The birth story of Sebastian Gordon von Frank

Tyrant Farms' articles are created by real people with real experience. Our articles are free and supported by readers like you, which is why there are ads on our site. Please consider buying (or gifting) our books about raising ducks and raising geese. Also, when you buy through links on our site, we may earn an affiliate commission. Learn more
On December 14, 2019 at 12:07am, our son Sebastian was born. This is his birth story.
We’re writing and sharing this story publicly for our own sake while the memories are still fresh and because some of the information may be helpful for other expectant parents out there.

Context: our birth goals and birth plan
Before diving in, a bit of context is necessary:
Every mother is different and every pregnancy is different. We’ll never judge another mother or parent who chooses a different approach to childbirth than the direction we chose and detail in this article. Other parents could easily make educated, informed, good-faith decisions that are entirely different than the choice(s) we made in our birthing approach.
We should also make it clear that we’re not spring chickens. We’re not quite geriatric, but we’re relatively high risk parents given our “advanced maternal and paternal ages,” 39 and 42 respectively. We had regular checkups throughout pregnancy and the only risk factor that showed up was a marginal cord insertion during a Week 23 ultrasound scan. (Oddly, a Week 38 scan didn’t show a marginal cord insertion.)
Why try for an unmedicated birth?
Our primary goal was to optimize the short and long-term health and wellbeing of both mom and baby. Trying for an unmedicated birth — assuming it’s a low risk pregnancy — is a great way to achieve that goal. An “unmedicated birth” simply means no labor induction, no epidural, and no C-section.
Notice we didn’t say “natural birth.” To us, “natural” doesn’t seem like an appropriate term to use unless the birth takes place out in a forest or meadow without modern conveniences. Hospital beds or birthing centers are not naturally occurring phenomena, and we’ve never seen fluid IVs growing in the wilderness.
The most commonly used medical intervention in the US is an epidural, which takes away the considerable pain of labor and pushing for mom. Epidurals are often an important and very necessary intervention.
However, as economist and research analyst Emily Oster (who is definitely not a hippy) details in her book Expecting Better, there are a number of increased risks associated with epidurals as documented by high quality research:
- Risks for baby: There’s a significantly increased risk of unnecessary antibiotics used on women/baby after an epidural. Epidurals often cause laboring women to run a fever, and since doctors can’t tell the difference between infection-induced fever vs epidural-induced fever, antibiotics are then used as a precaution. Since one of the newly discovered benefits of vaginal delivery is the introduction of beneficial microbes/bacteria that help inoculate baby’s microbiome and charge up their developing immune system, antibiotics may well kill off many of the beneficial organisms that assist in that critical process.
- Risks for mom: Via Emily Oster: “Greater use of instruments (forceps or vacuum in delivery), greater use of C-section for fetal distress, longer pushing time (15 minutes), higher chance of baby facing up at birth, greater use of Pitocin in labor, greater chance of low maternal blood pressure, less able to walk after labor, greater chance of needing a catheter, increased chance of fever during labor.”
So our desire for an unmedicated birth wasn’t due to heroism or the belief that mom should suffer terrible pain for her baby. Rather it came from wanting the best possible health outcomes for all involved while trying to prevent the domino effect that often comes once medical interventions start.
What are the benefits of using a midwife?
We chose to have a midwife-led birth rather than a birth led by an OBGYN. (We also took a midwife-led Centering class and a separate Lamaze class from an excellent doula, Jen Hutchison.) These childbirth classes took away a lot of the unknowns, uncertainties, and fears we had going into birth as first-time parents, and we’d highly recommend them to other would-be parents.
Certified nurse-midwives (CNMs) are highly educated, trained, and credentialed nurses/birth experts who tend to take a more holistic approach to childbirth, helping to educate parents in detail about what to expect throughout the entire pregnancy and birthing process. They also encourage women to aim for reduced medical interventions during childbirth, if possible. Midwives are with you at the end to deliver your baby and do the best they can to balance between your birth goals going in to delivery with your/your baby’s health when the day (or days) of labor and childbirth finally come.
We had the best of both worlds via Prisma, our local hospital system: a midwife-led birth inside the maternity ward at our hospital. If something went wrong, there’d be additional medical professionals and technologies there to assist. All we had to do was get to Active Labor (3-7 centimeters dilated) at home, then call our midwifery to let them know we were on the way to the hospital. Piece of cake – ha!
If midwife-led pregnancies were the norm for low-risk pregnancies in the US (as they are in many European countries), the US could drastically reduce our astronomically high childbirth costs and likely improve health outcomes as well. Many people don’t realize that it costs far more to deliver a baby in the US than any other country, despite the US being the most dangerous developed country in the world in which to give birth.
As a recent article in Scientific American notes:
“Studies show that midwife-attended births are as safe as physician-attended ones, and they are associated with lower rates of C-sections and other interventions that can be costly, risky and disruptive to the labor process.”
Ok, now that you have necessary context for our birthing goals and decisions, you’ll have context for the birth story of our son, Sebastian…
Dr. Lisa (aka Susan’s sister) comes to help
Susan’s sister Lisa is one smart and tough cookie. She’s a nationally recognized child and adolescent psychiatrist, a mom, and the medical director of her own mental health practice in Las Vegas, Nevada. She’s also a five-time cancer survivor — yes, seriously! (Susan was adopted into the family, so they do not share the same genetic risks.)
Lisa and The Tyrant are very close, so Lisa offered to fly out to be here for us and assist us through the birthing process. Two decades ago, she completed her medical residency at the same hospital system here in Greenville, SC, where we planned to give birth. During her residency, she delivered 13 babies on the same hospital floor where we’d be giving birth to Sebastian.
She bought plane tickets and planned to stay with us for one week prior and one week past our due date, given that only about 5% of births happen on the actual estimated due date.
During the first week after Lisa’s arrival we all had a great time. Lots of laughing, making meals together, and taking walks on the Swamp Rabbit Trail (Susan walked 2-3 miles per day during the last weeks of her pregnancy).

Who would catch baby?
Another thing we discussed: who would “catch” baby Sebastian when he entered the world: me, Lisa, or the midwife? Considerations:
- Susan wasn’t sure how she felt about me being “down there” during the birthing process (nor was I).
- I had no idea how I’d react to seeing the goings on down there or whether I’d still be standing when the time came to actually catch our baby.
- My main objective was comforting and encouraging Susan throughout labor, which meant I would be spending a lot of time at her head end, not her tail end.
- Lisa wanted to catch the baby if we were open to it.
We ended up deciding that I’d stay away from the “business end” and Lisa would get to catch her fourteenth baby (but the first one in her family). Since Susan is adopted, Sebastian would be the first and only genetic relative she’d ever known, and she liked the idea of her big sister welcoming Sebastian into the world, just as Lisa welcomed her when she was a baby.

Dec 10 due date arrives and passes
Right around our due date (Dec 10), Lisa found out she would have to cut her trip short and fly home on Sunday, Dec 15th due to family and business emergencies. Things really needed to get going if she was going to be there for the birth and help us during the difficult transition to baby care immediately after birth. Plus, she was the one designated to trek home to look after our ducks while we were in the hospital, and we didn’t have a backup duck sitter lined up.
We didn’t chart incoming phone calls and text messages from parents, but they seemed to increase markedly the closer we got to the due date, then another ten-fold once our due date passed. “Any news yet?” “How are things going today?” (For the record, our parents have been wonderful and caring throughout each step of the process.)
Needless to say, we felt the pressure and stress increase the further past our due date we got and the closer we got towards Dec 15th when Lisa would have to leave. There was also the concern of increased neonatal health risks if we got to Week 41 of pregnancy. At that point, even midwives will encourage you to consider medicated induction (via pitocin) to get the baby out asap before anything bad can happen inside due to increased risks.
On December 11th, we went to the midwifery for our regular weekly checkup. We also had a non-stress test performed to have a long listen to baby’s heartbeat, mom’s uterine contractions, and the interplay between both measurements (abnormalities, baby’s stress response to Braxton Hicks contractions, etc). Result: baby and mom were both healthy… but no signs of labor.
By the 12th, Susan was beyond done with being pregnant. Lisa was getting stressed out and encouraging us to consider an induction to reduce health risks to baby. In her practice, she sees kids who endured all sorts of lifelong horrors due to births that did not go according to plan.
Friday 13th
Then Friday 13th came… Everybody knows this to be a date of dread and bad luck in western culture (although nobody is quite sure why). We’re far from superstitious, but we weren’t thrilled about giving birth on this day, even if it meant Lisa won the $0.25 family bet of what date the baby would be born.
We decided we were going to do every trick possible (even silly stuff) to trigger spontaneous labor, short of animal sacrifice (which our ducks would NOT approve of).
The day prior, Susan and Lisa went to a Chinese foot spa to see if that could magically induce spontaneous labor (not evidence-based). No luck. Immediately after, she started doing “nipple stimulation” via her breast pump, which is also supposed to trigger hormonal responses to induce spontaneous labor. No luck. Spicy dinner? Nope, no luck.
On the morning of the 13th, Susan had a cervical sweep at our midwifery, which she described as extremely unpleasant. (Some women say the procedure is as bad as labor.)
After the cervical sweep, we went to the store to get ingredients for the notorious “midwive’s brew,” which is consumed by full term moms-to-be to induce spontaneous labor. Most of the ingredients in midwive’s brew are designed to mask the taste of the horrible tasting ingredient that’s been proven to safely trigger uterine spasms and ultimately contractions: castor oil.
We ate lunch, watched Susan drink her midwive’s brew, and waited. The immediate result? Nothing beyond some Braxton Hicks contractions, which she’d been having for over a month.
Dinner time
I performed evening duck duties, which includes bringing two of our duck, Jackson and Marigold, inside for the night. Lisa prepped a light dinner since Susan wasn’t feeling great.
We began eating dinner around 7pm. Then Susan’s water began to break and she experienced a new sensation that was beyond the standard Braxton Hicks contractions: early labor. Not comfortable, but not the most painful thing she’d ever felt. Finally!
I texted my parents at 7:50pm (with Lisa cc’d) to let them know that we were going into labor and I’d be out of touch since my focus would be exclusively on Susan with zero distractions. Lisa would keep them updated as things progressed. (We expected labor to go well into Saturday and even Sunday based on stats for first time moms.)
In pop culture and movies, mom’s water breaks and she rushes to the hospital. In reality, many/most women don’t have their water break until long after labor starts. Another fallacy that gets presented is that labor starts, you rush to the hospital, and then you’re holding your baby a few minutes later.
The reality is that the First Stage of labor can easily last for 24+ hours and mom’s water might not break at all during that time window. Over that time period, a woman’s cervix very slowly widens and thins (dilates) with each contraction, eventually reaching 7 centimeters dilated at which point she’s typically been laboring for a looong time so she’s more acclimated to the intensity of impending Transition contractions (7-10 centimeters dilated). This is the point when you call your midwife and the earliest point at which a hospital will admit you. And these were the birthing expectations we were prepared for…
Going from zero to Transition in record time
Susan got into a nice warm bath at home and settled in for a long, slow night of Early – Active labor. We started timing contractions on our pregnancy apps so that we’d know for certain where we were in the process and when it was time to call the midwife and head to the hospital.
All was going according to plan for about 30 minutes. Then around 9:15pm Susan heard and felt a pop sound in her abdomen, followed by extraordinarily strong abdominal pain and a contraction that made her scream, weep, and get wobbly-knee’d.
Lisa went into doctor mode; I rushed our indoor ducks out to the outdoor duck coop since we’d potentially be gone for days with no duck sitter. By the time I came back inside, Lisa was on the phone with our midwife and Susan was bowed over the bed screaming in pain. Things were not going according to schedule or plan or anything else we had envisioned.
For a bit of context, Lisa describes Susan as having an unusually high pain tolerance. Typically, a prolonged Early – Active labor period gives mom’s body and mind a chance to acclimate to the super-human levels of pain experienced during Transition and Pushing. Somehow, Susan seemed to skip right over Active Labor and go right to the excruciating point of Transition, with no acclimation period.
To the hospital
The 15 minute ride to the hospital was not a pleasant one. Susan was in the passenger seat trying to take deep breaths as calmly as possible between 2-3 minute contractions. The contractions were so intense and painful I could feel her whole body shaking uncontrollably as I held her hand. “I don’t think I can do this,” she shrieked.
Lisa was in the back seat and we both tried our best to talk Susan through each wave of tortured pain.
I pulled up in front of the hospital, rushed in to grab a wheelchair, then rushed back out to get Susan. I swept her inside while Lisa parked the car. (Side note to Prisma Health: please get wheelchairs with a luggage chamber on the back — I’m fairly strong and even maxed out on adrenaline had difficulty pushing Susan with one hand and carrying a suitcase with the other.)
I quickly got Susan up to the 6th floor, through maternity admittance, and into her L & D triage room. A nurse talked to us for a couple of minutes until Barb, our midwife-on-call, showed up. At this point, contractions were so extreme that Susan couldn’t support herself. She was leaning over the hospital bed wailing through each contraction and she screamed for Barb to please help her. I could feel her body trembling in agony as I tried to hold and console her.
She couldn’t bear it. She told me and Barb that she needed an epidural immediately, and we both were happy to oblige. After all, it’s her body and her experience to endure – the rest of us are supporting characters. I asked her if she was sure because I knew going in, she wanted to have an unmedicated birth. Barb also asked her if she was certain she wanted an epidural because she was an excellent candidate for waterbirth, which was part of her initial birthing plans as well. “Yes, I’m done,” Susan responded firmly and clearly.

Then Barb checked her cervix and told us the surprising news: “You’re already at 8 centimeters dilated. We’re going to take you to the delivery room now.” Lisa had just arrived to the room.
We all raced behind the rolling hospital bed shouting words of encouragement as Susan screamed through each contraction. The halls seemed labyrinthine in their construction. Each time I thought we’d reached the final hall or turn, we kept going.
Finally, we made it into our delivery room where a team full of nurses was waiting for us. It had only taken a few minutes to go from triage to our new room, but now Susan was at 10 centimeters dilated, which is when the urge to push becomes overwhelming. They hooked her up to a fluid IV but let us know that there was no point in doing an epidural: by the time they hooked up the system and the pain medication took effect, the baby would likely be here. We were going to have a medication-free birth after all, whether we wanted it or not.
I remember feeling horrified and helpless that the person I love more than anything in the world was in so much pain and there was nothing I or anybody else could do to stop it. At this point in the birthing process, hormones kick in to send moms into something of an altered state of consciousness.
Susan obeyed her body’s urges to start pushing. In unison, the midwife and nurses gave her clear instructions of when and how long to push. I held Susan’s hand, stroked her face with a cool wash cloth, and kissed her head, whispering my love and encouragement into her ears as each minute wore on.
The experience was so extreme and overwhelming that all sense of time melted away. Were we minutes in? Hours? I had no idea. As things progressed, they put an oxygen mask on Susan’s face. (We came to find out later this was in response to the baby’s vital signs which they were monitoring plus Susan’s potential of going into shock.)
Finally, after what seemed like hours of pushing, I heard Lisa and the midwife excitedly exclaim, “look at that little hairy head!” There was a finish line. A few more pushes and I heard a splattering of fluids followed almost immediately by a distinct high pitch cry. Our baby was born.
At 12:07am on December 14, Lisa caught her 14th baby in the same hospital she’d learned to be a doctor in, only this one was her sister’s baby. However, since Sebastian wasn’t born on Friday 13th, she would have to fork over $0.25.
Susan sunk back in bed, exhausted. “You did it. You’re amazing,” I told her. She’d pushed so hard that capillaries had burst all over her face (a condition which goes away within a couple weeks after pregnancy).
I remain completely in awe of what her mind and body endured, which is wholly beyond my linguistic capacities to articulate.
Moments later, Lisa placed Sebastian on Susan’s chest.

We both started speaking to him; his eyes were clear and vibrant. He seemed to recognize our voices, the voices that had spoken to him throughout his development. The voices that read to him lovingly each night through a delicate wall of mom.

Within 15 minutes of birth, Sebastian made a good latch and was comfortably seeking out his first meal of colostrum: the protein dense probiotic and antibody-rich milk that comes before mom’s regular milk fully arrives a few days later. Yet another female superpower.
A short while later, Susan and I were transferred from the delivery room to our in-patient room with our son. Three of us.


From there on, a lifetime of new stories begins, and our story will never be the same. Sebastian Gordon von Frank was born, a first name that speaks to something new and all his own with middle and last names that pay tribute to the loving families who taught us what family is all about.
We’re overwhelmed with gratitude as we start to write the new chapters of our family’s life. We’re also overwhelmed with love for our son.
And so life begins, anew…
A few photos of baby Sebastian



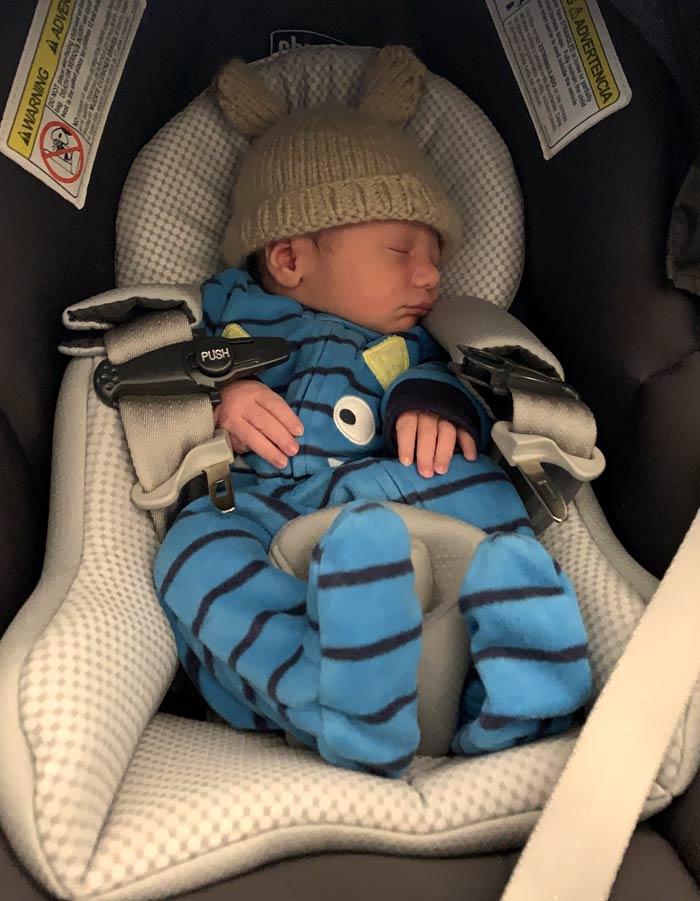


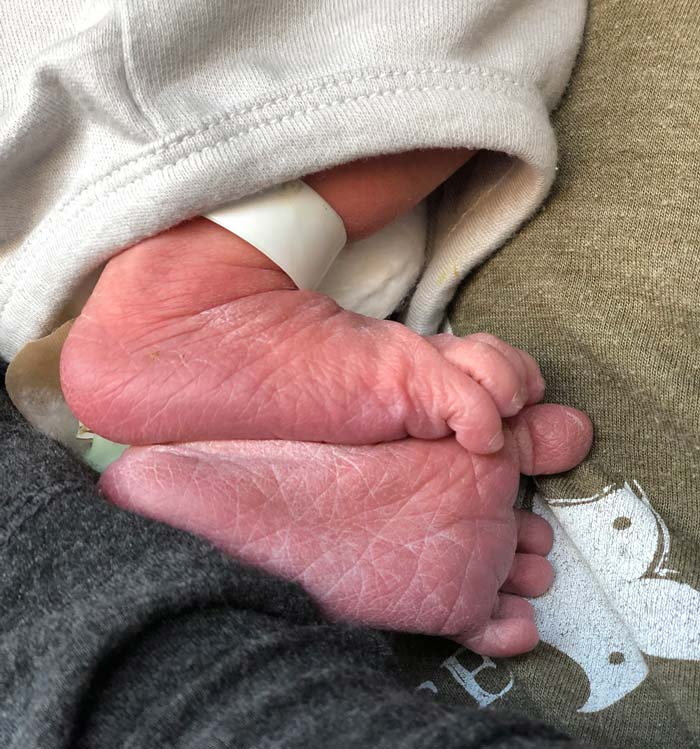
Was this story helpful or interesting?
Please share it and browse our other parenting articles!





I just bawled reading this, brings back so many emotions from when I became a mom. Thank you for sharing your story.
You’re very welcome. Glad the story helped you reconnect to your own birth memories and emotions. It’s a magical experience.
Welcome Sebastian! So nice to read this story, and hear you were born on one of my brothers’ birthdays 🙂 My best to all of you ❤️
Thank you, Cecile!
Thank you!